Transcranial Magnetic Stimulation | Vibepedia
Transcranial Magnetic Stimulation (TMS) is a noninvasive medical procedure that employs focused magnetic fields to modulate neural activity in specific brain…
Contents
Overview
Transcranial Magnetic Stimulation (TMS) is a noninvasive medical procedure that employs focused magnetic fields to modulate neural activity in specific brain regions. By inducing electrical currents in targeted cortical areas, TMS offers a novel approach to treating a range of neurological and psychiatric conditions. While its efficacy for conditions like major depressive disorder (MDD), obsessive-compulsive disorder (OCD), and chronic pain is increasingly recognized, debates persist regarding optimal protocols, effect sizes, and the significant role of placebo responses. The technology, rooted in early discoveries of electromagnetism, has evolved from experimental research tools to FDA-approved therapeutic devices, marking a significant advancement in neuromodulation techniques.
🎵 Origins & History
The genesis of transcranial magnetic stimulation traces back to the late 19th century with the foundational work on electromagnetism by scientists like Michael Faraday and James Clerk Maxwell. However, the direct application to human brain stimulation began to emerge in the early 1980s. The first functional TMS device was initially used for motor cortex mapping. This breakthrough allowed for non-invasive stimulation of neural pathways, differentiating it from earlier, more invasive techniques. The subsequent decades saw rapid refinement of coil designs and pulse parameters, paving the way for therapeutic applications beyond research, notably for depression and neurological disorders.
⚙️ How It Works
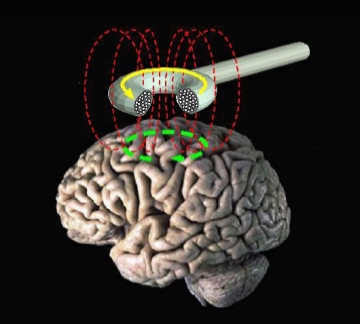
At its core, TMS operates on the principle of electromagnetic induction. A TMS device, typically comprising a pulse generator and a magnetic coil, delivers brief, powerful electrical currents to the coil. This rapid current change generates a transient magnetic field that penetrates the skull with minimal attenuation. As this magnetic field passes through the brain tissue, it induces a secondary electrical current in the neurons within a targeted region. This induced current can either depolarize neurons, increasing their firing rate, or hyperpolarize them, decreasing activity, depending on the stimulation parameters and the specific brain area targeted. The precise modulation of neural circuits is the key mechanism underlying its therapeutic effects, influencing neurotransmitter release and synaptic plasticity.
📊 Key Facts & Numbers
The typical treatment course involves daily sessions for 4-6 weeks. The FDA has approved TMS devices for treating major depressive disorder (MDD) in adults who have failed to achieve satisfactory improvement from prior antidepressant medication, as well as for obsessive-compulsive disorder (OCD) in adults and adolescents aged 12 and older. Studies suggest that approximately 50-60% of patients with treatment-resistant depression experience significant symptom reduction, with about one-third achieving remission. The typical treatment course involves daily sessions for 4-6 weeks, totaling 20-30 sessions.
👥 Key People & Organizations
Key figures in the development and clinical application of TMS include Anthony Barker, the pioneer of the technology. Organizations like the U.S. Food and Drug Administration (FDA) play a crucial role in approving TMS devices for specific medical indications. Major manufacturers of TMS equipment include Magstim, Brainsway, and Neura Performance, each contributing to the technological advancements and market availability. Numerous research institutions and university hospitals, such as Yale University and Stanford University, are at the forefront of clinical trials and research into novel applications of TMS.
🌍 Cultural Impact & Influence
TMS has significantly influenced the landscape of psychiatric and neurological treatment paradigms, offering a non-pharmacological alternative for conditions previously managed primarily with medication or electroconvulsive therapy. Its non-invasive nature has reduced the stigma associated with brain stimulation therapies and increased patient acceptance. The technology has also spurred innovation in related neurotechnology fields, influencing the development of other neuromodulation techniques like deep brain stimulation and transcranial direct current stimulation. Public awareness has grown through media coverage and patient testimonials, contributing to its increasing adoption in clinical practice.
⚡ Current State & Latest Developments
The current state of TMS technology is characterized by expanding indications and refined protocols. Ongoing research is exploring its efficacy for conditions such as post-traumatic stress disorder (PTSD), schizophrenia, Parkinson's disease, and stroke rehabilitation. Companies are developing more portable and user-friendly TMS devices, aiming to increase accessibility. Furthermore, advancements in artificial intelligence and machine learning are being integrated to personalize TMS treatment parameters for individual patients, optimizing outcomes.
🤔 Controversies & Debates
A central debate surrounding TMS revolves around its efficacy and the magnitude of its therapeutic effects. While studies consistently show that TMS is more effective than sham treatment for MDD, the effect sizes are often modest, and placebo responses can be substantial, sometimes accounting for a significant portion of the observed improvement. This has led to ongoing discussions about the optimal stimulation parameters, target areas, and treatment duration. Another controversy concerns the potential for adverse effects, though serious adverse events like seizures are rare. The cost of TMS treatment and insurance coverage also remain points of contention, impacting patient access.
🔮 Future Outlook & Predictions
The future of TMS appears bright, with projections indicating continued growth and diversification of its applications. Researchers are investigating the use of theta-burst stimulation (TBS), a more rapid form of TMS, which could potentially shorten treatment times and improve patient compliance. Integration with neuroimaging techniques like fMRI is expected to enable even more precise targeting of brain regions. Expansion into new therapeutic areas, such as addiction treatment and autism spectrum disorder, is also on the horizon. The development of closed-loop TMS systems, which adjust stimulation in real-time based on brain activity, represents a significant frontier.
💡 Practical Applications
TMS has found direct application in treating several clinical conditions. For major depressive disorder, it is used to stimulate the dorsolateral prefrontal cortex, an area often hypoactive in depressed individuals. In obsessive-compulsive disorder, stimulation of the medial prefrontal cortex and anterior cingulate cortex is employed. Beyond these FDA-approved uses, TMS is being explored for chronic pain management by targeting somatosensory cortex regions, and for stroke rehabilitation to enhance motor recovery by stimulating the motor cortex. It also serves as a valuable tool in neuroscience research for mapping brain function and understanding neural circuits.
Key Facts
- Category
- technology
- Type
- technology